If we are in an accident or have an operation and lose blood, we take it for granted that we will be given a transfusion. Not only that, but it will be matched to our blood type, will have been stored in the correct conditions and will be delivered using sterilised equipment to avoid infection.
At the start of the First World War blood transfusion technology was largely untested and not widely accepted. Blood types had first been identified at the turn of the century, but where transfusions were carried out surgeons did not test the blood for compatibility. This could be fatal where the patient’s immune system attacked the new blood cells.
Transfusions were ‘direct’ using a tube to carry blood from an artery in the donor to a vein in the patient – this carried the risk that blood would clot and block the tubes. As is so often the case in war, new techniques were advanced in the urgency of the battlefield, and in this case, a Canadian, an American and an Englishman all played vital roles.
The Canadian was Lawrence Bruce Robertson. Of Scottish background, Robertson was born in 1885 in Toronto. He joined the Canadian Expeditionary Force and was posted to the Canadian Army Medical Corps’ No. 2 Casualty Clearing Station. He persuaded the British surgeons at the casualty clearing stations to practice ‘indirect’ blood transfusions, where blood was transferred using syringes and canulae to overcome problems of clotting – a technique he had used at Toronto’s Hospital for Sick Children.
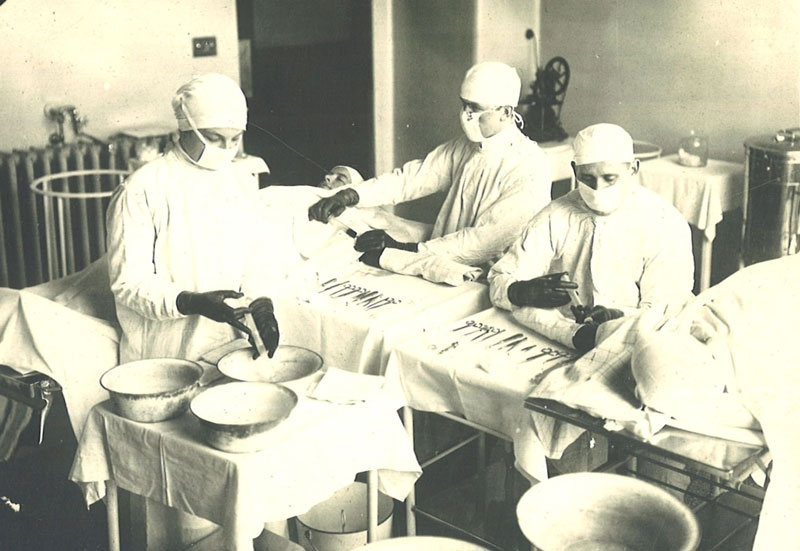
Blood transfusion procedure, 1918. Reproduced with kind permission of the Hospital Archives, The Hospital for Sick Children, Toronto, Canada
Robertson set up the first blood transfusion equipment at a casualty clearing station on the Western Front in Spring 1917 and began to record the results of the transfusions he performed. In an article in The Lancet published on 24 November 1917, Robertson described 36 cases where he had used the indirect transfusion method. He wrote that ‘In the cases of severe primary haemorrhage accompanied by shock, blood transfusion frequently produces an immediate and almost incredible improvement. The change from a pallid, sometimes semi-conscious patient with a rapid flickering pulse to a comparatively healthy looking conscious and comfortable patient with a slower and fuller pulse is dramatic evidence of the value of the transfused blood.’
Robertson’s article in the Lancet was printed with a note by Colonel Charles Gordon Watson, the consulting surgeon to the British Expeditionary Force, which said ‘During the past year I have had the opportunity of observing the technique and the results of blood transfusions by Major Bruce Robertson and other workers. Without doubt transfusion of blood after primary haemorrhage is a life saving device of the greatest value and enables urgent operations to be successfully performed under conditions otherwise hopeless.’
Another Robertson, this time an American by the name of Oswald Hope, played an equally important role in developing blood transfusion technology. Oswald Robertson was born in England in 1886 but emigrated to America as a child. He qualified as a doctor in 1915 and joined the Western Front as a volunteer with the United States Army, attached to the 48th casualty clearing station. He built the world’s first blood bank – storing blood mixed with a citrate and dextrose solution in glass bottles kept on ice. The blood could be kept for up to 26 days and moved to casualty clearing stations ready to be used in transfusions to patients.
In an article in The Lancet published on 22 June 1918, Robertson described the technique and equipment to be used in storing blood safely for later use. He discussed the results of blood transfusions using stored blood saying that ‘The effect of transfusion with preserved blood was fully as striking as that observed after the giving of freshly drawn blood. There was the same marked improvement in colour, the pulse became slower and stronger, and the blood pressure showed an increase of 20 to 40 points’.
During heavy fighting a casualty clearing station received many seriously wounded men at once. The less seriously wounded, who would normally have been able to donate blood, were not taken to the casualty clearing stations. This meant that having a stock of stored blood allowed the medical services to give transfusions quickly and easily. Robertson was awarded the Distinguished Service Order by the British Government in recognition of the lives his techniques had saved.
Another aspect of blood transfusion technology was developed by an Englishman, Geoffrey Keynes. Born in 1887, Keynes qualified as a surgeon with the Royal College of Surgeons in London and in 1917 he married Margaret Darwin – granddaughter of Charles Darwin.
Like many other doctors, Keynes was granted a temporary commission with the Royal Army Medical Corps. His medal card (WO 372/11/152014) shows he was attached to the 4th General Hospital. Service records for RAMC officers who received a permanent commission are at The National Archives in WO 339, but service records of officers with a temporary commission for the duration of the war were destroyed after 1920. War diaries of hospitals and ambulance trains in WO 95 can sometimes mention officers by name and illustrate the day to day experiences of those who served with the RAMC.
Keynes developed equipment that enabled blood transfusions to be carried out away from established medical facilities. Where there was no refrigeration available to store blood, the best hope a patient had was to get a transfusion there and then from another person. Keynes’ equipment enabled ‘indirect’ transfusions by regulating the flow of blood between the donor and the patient.

Mobile blood transfusion equipment devised by Geoffrey Keynes. Reproduced with permission of Science Museum/Science & Society Picture Library
It’s difficult to imagine how many men must have owed their lives to the techniques developed by these three men. Thanks to their skills and inventiveness, blood transfusion became accepted practice within the Royal Army Medical Corps which later declared it the most important medical advance of the war.


My grandad was instrumental in saving the life of a soldier at the 2nd. Canadian Casualty Clearing Station, under Dr. Robertson, by donating blood in 1916. He was a gunner in the British artillery. When in Guildford recovering from hernia surgery, grandad wrote a thank you letter to Dr. Robertson for his care, it is now in the National Archives in Canada, with other papers of the doctor’s. I found it on the website of the Archives, and was able to tell my mom about it while she was alive, she was thrilled. Would love to see the actual letter as I knew my grandad briefly when I was little. Have a copy of it, though.
And all of this was also thanks to Luis Agote who made the first anticoagulated blood transfussion in 1914.